AL man spent weeks in a coma after COVID diagnosis. God ‘didn’t have to wake me up,’ he says
The entry hallway at River Towne Care erupted into applause as Eric Lofton turned the corner to be discharged from the Columbus nursing care facility.
Staff members filled the foyer, holding handmade signs and a large poster board that they had signed with messages for Lofton. The artist behind the signs, River Towne’s activity director Julia Taylor, pushed Lofton’s wheelchair out of the front doors on May 27.
She said she wanted it to feel “almost like a wedding,” a celebration of Lofton’s respiratory recovery.

Jenny Phillips, Lofton’s girlfriend, tossed his bags into the back seat, helped him into the car and stuck the keys in the ignition as a few workers trickled out of the building to say a final farewell.
Five months ago, Lofton, 45, had been diagnosed with COVID-19 and placed on a ventilator for five weeks. After two months of recovery at the Columbus nursing facility, he’s ready for the drive back home to Enterprise, Ala.

From coronavirus to pneumonia to a coma
On Dec. 31, 2020, Lofton had a heart attack and was admitted to the hospital for three days.
The next week he was diagnosed with COVID-19. A week after that, pneumonia. He was sent home with steroids.
Lofton has previous medical diagnoses that makes coronavirus even deadlier: congestive heart failure, atrial fibrillation and high blood pressure.
Before being diagnosed, Lofton said he’d been “skeptical” of the COVID-19 pandemic. He said he didn’t interact with many people day-to-day, especially in his job as a truck driver.
He watched news reports saying people young and old were dying from the virus. Lofton knew it was a a threat, “but I guess I was thinking I was one of those people that wouldn’t catch it,” he said. “I take it as a more serious thing than I did before.”
On February 3, Lofton couldn’t catch his breath. He was admitted to the Southeast Medical Center in Dothan, Ala., where he was immediately sedated.
“And that’s when I fell into a coma,” he said.
Hospital staff would later tell Lofton that his mother, Jenese Florence, called often. That’s how she learned her son had been placed on a mechanical ventilator for five weeks.
“Usually when you get on a ventilator, the odds aren’t good for you,” said Mark Stewart, the Director of Public Relations for the East Alabama Medical Center.
A ventilator doesn’t treat COVID, but rather supports the body as it fights off infection by delivering oxygen to vital organs via a breathing tube to the lungs.
When Lofton woke up from his coma on March 2, he had a tracheostomy tube in his throat. He thought he was in another state, describing a mental fuzziness that lingered for weeks.
He could move his legs while lying in bed. Certain he could walk, he asked nursing staff to bring over a chair so he could stretch his legs.
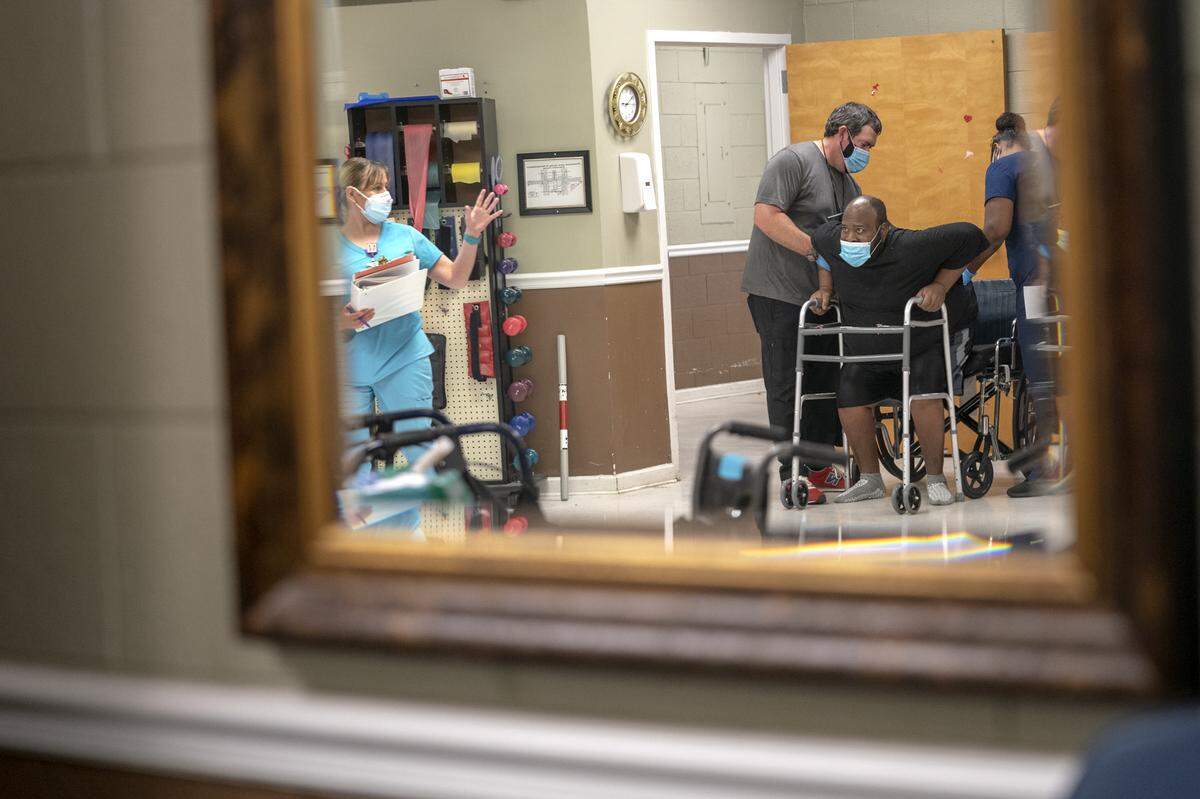
Lofton thought he would “catch a bus and go home.” But when he stood up to get into the lounge chair, his legs gave out and five nurses had to help him regain his balance.
A disconnect was present after he awoke from the coma — before January, Lofton was fully capable of walking and caring for himself. Now, he had very little mobility and remained isolated in the COVID ward at the hospital.
The following month was a challenge. Lofton struggled to remember names, experienced vivid nightmares and forgot phone calls he’d had with family members the day before.
Lofton said his brain fog made it difficult to discern dreams from reality. He’s a single father and recalled that in one dream, he thought his 16-year-old daughter had died. He didn’t have access to a phone to call her.
“I’d been gone from my family for so long,” Lofton said.
A week later, his mother visited and assured him the family was OK.

On April 2, Lofton’s case manager secured a spot at River Towne nursing home in Columbus to begin respiratory therapy. His first glance at the city in years was a blur of highway and passing cards through the ambulance window, he said.
Respiratory care facilities hard to find
In southeast Alabama, there were no nearby respirator rehabilitation centers to help Lofton. River Towne was the closest facility — 115 miles away from his home in Enterprise.
River Towne is equipped with 23 ventilator units and a team of 16 respiratory therapists to provide ventilator recovery. The facility is split between respiratory care and rehabilitation. Lofton needed both.

Ida Batson, respiratory director at River Towne, said she has helped five patients recover from a ventilator in the last 10 months.
There are at least 10 more people on a waiting list, Baston said. Each case requires an enormous amount of attention, she said, and access to equipment and insurance are the largest barriers to accepting new patients.
River Towne has provided respiratory services for three years but experienced a “huge increase” in demand since March 2020, said Batson.
The first time Batson met Lofton, she asked him if he planned to permanently live at River Towne. The answer was a resounding no. He told her he wanted to be out of the care facility by May 31.

“OK, then you’ve got to do the work,” Batson recalls telling Lofton. “You’ve got to get yourself out of bed.”
He would eventually beat his goal by four days.
“I told my therapists, ‘this guy is not going to be here long. We’re going to get him out of here,’” Batson said.
Ready to ‘get back out’
When Lofton’s trach tube and ventilator were removed, his body had to learn to breathe on its own. Intense physical therapy helped him swallow, speak, breathe and get around with a walker. His labored breathing and coughing have subsided over the last couple of months.
Lofton speaks softly, intentional with his words but the first to crack a joke with his occupational therapist.
“Are you showing off?” she chuckled during one recent session. Lofton was tossing cones behind his back, an exercise in flexibility. He’d just mastered two laps around the room with his walker.
Placing the last cone on the table, he responded quickly, “Now you know I’m always on this level.”
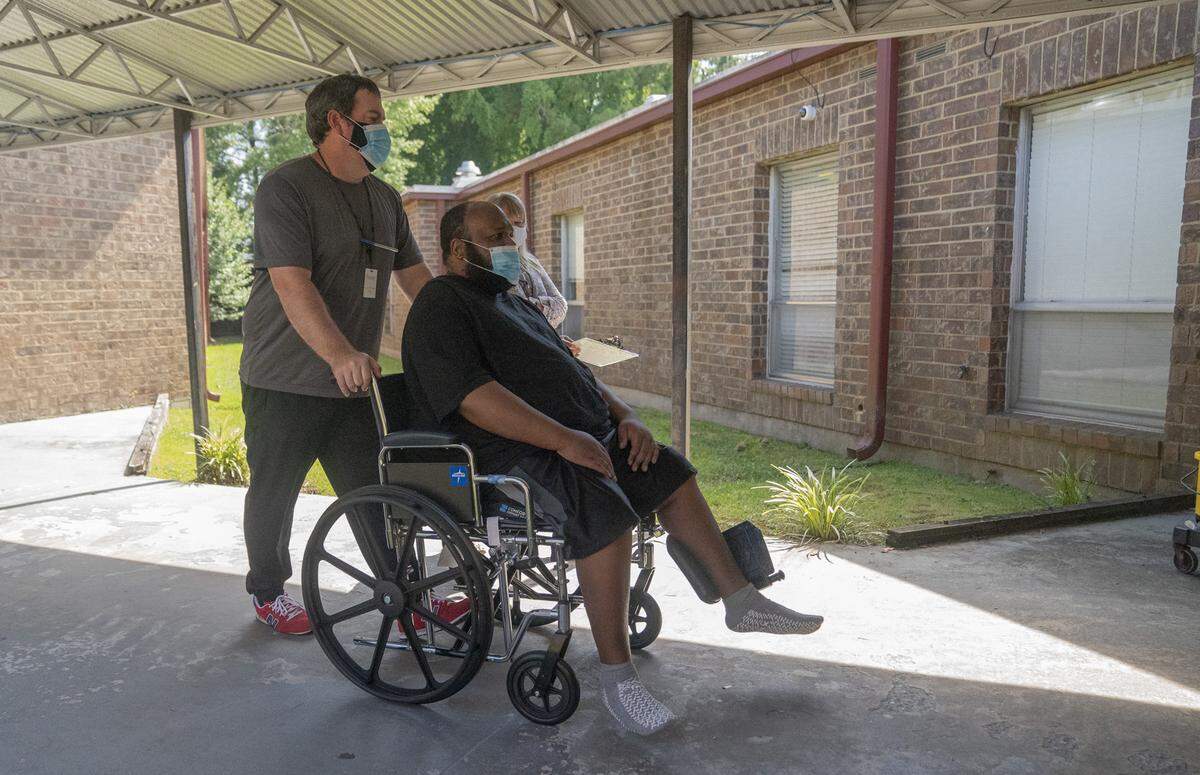
Working with occupational and physical therapists, Lofton progressed. His exercises included bouncing a ball, squats, using a walker and riding on a bike machine.
“Some days, I don’t quite make it,” he said, but his body again feels more like his own.
In downtime between sessions, Lofton kept himself busy watching the news and calling family. “When you been in the outside world for so long, you want to get back out,” he said.
After spending almost two months at River Towne, Lofton met the threshold to be discharged. He can breathe on his own, get in and out of bed and eat a normal diet.
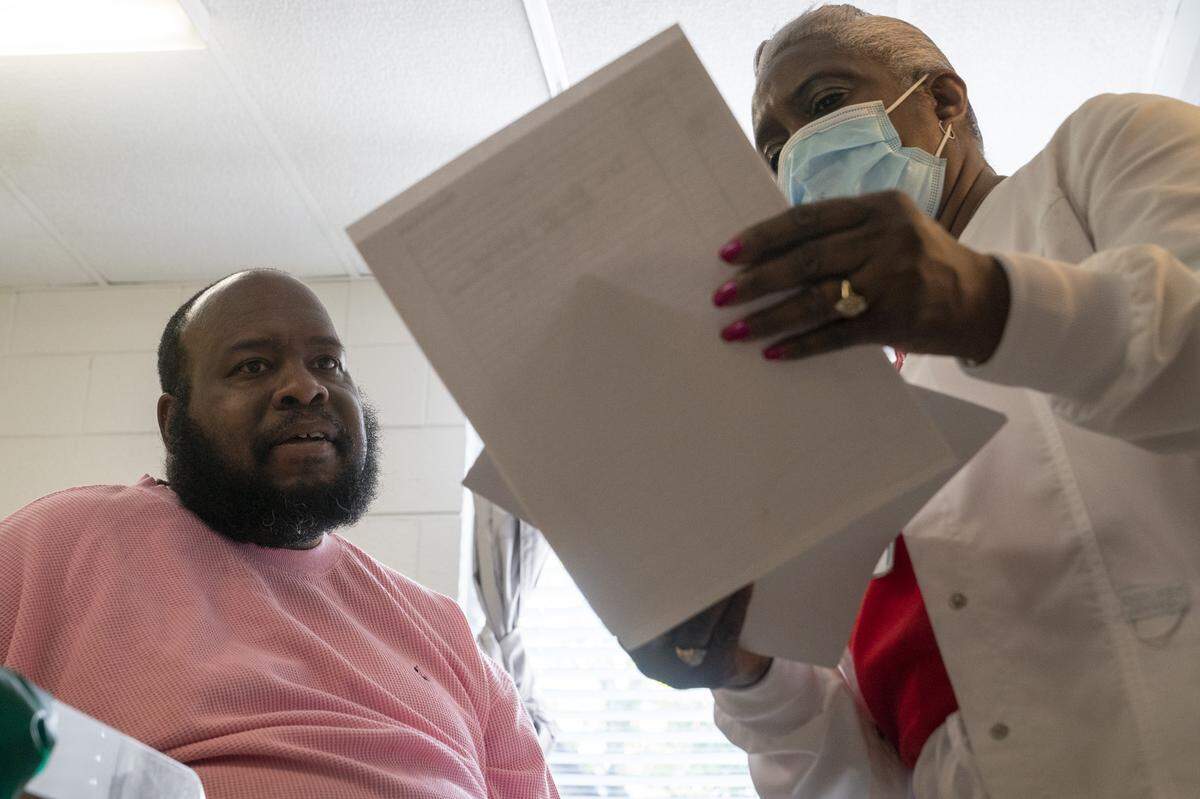
River Towne staff also observe a patient’s mental health carefully throughout rehabilitation. It can be a major obstacles to being released, said Batson. Patients recovering from mechanical ventilation have higher rates of PTSD, anxiety and depression.
“He didn’t have to wake me up,” Lofton said, crediting his faith in God for getting him through the past five months. “But it was also having faith in the people that are (at River Towne).”
There isn’t an average recovery time for a ventilated patient, Batson said. Some need a week to recover, others up to six months.

Lofton can’t wait to get home, visit church and eat his “mom’s home cooking.”
When he returns to Enterprise, a nurse will visit three times a week to help with physical rehabilitation. Before leaving, Lofton ordered gym equipment that he’ll set up in his kitchen.

Batson said she’ll miss seeing Lofton in the hallways. “He will not let me walk by his room without saying hi,” she said, describing Lofton as an “exceptional patient.”
“We want him to go home knowing he’s made an accomplishment,” she said. “ He survived something a lot of other people haven’t.”

Emotional goodbyes on discharge day
On his way out, River Towne staff cheered on his recovery and handed him notes of encouragement. As he and his girlfriend set off for Enterprise, Lofton held a yellow sign that read “Keep Smiling!”

He didn’t need to read the note to remember. He grinned at every person waving him goodbye as they drove away to his mom’s house. She visited nearly every week, but Lofton was elated to be the one finally going to see her and his daughter.
Throughout his rehabilitation, Lofton said his family kept him grounded. They also helped him pay most of his medical costs but after five months of intensive treatment, his savings are drained. Heading home, he knows his apartment rent is “behind significantly” along with other household bills.
Lofton said he’ll apply for disability until he is mobile enough to begin looking for another truck route.
One of the first things he’ll do when he gets home? Get vaccinated. “I know it’s been hard on some people to wear a mask... but we have to if we haven’t been vaccinated,” he said. “Everybody needs to take it as being serious.”
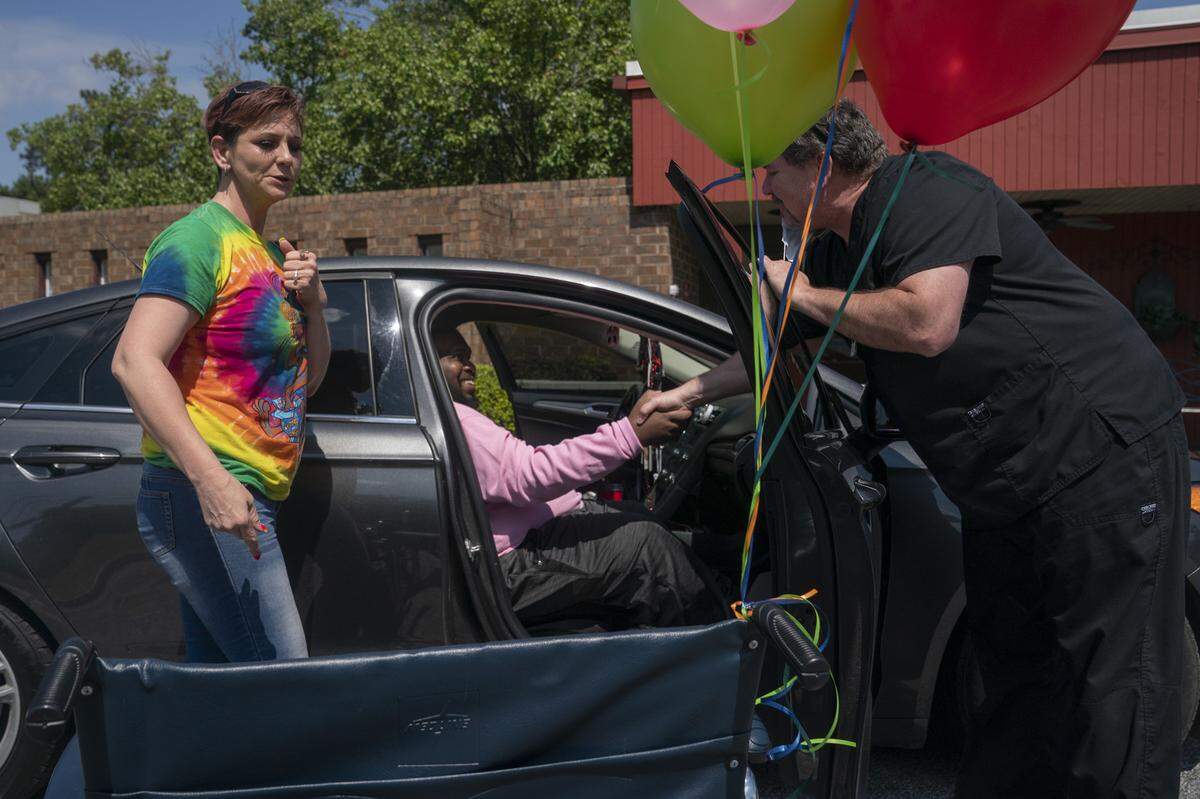
This story was originally published June 5, 2021 at 7:00 AM.